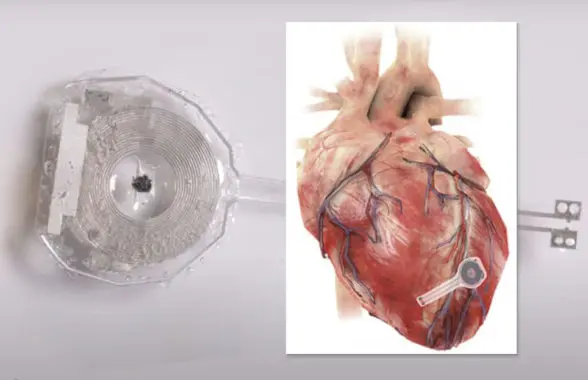
Scientists at Northwestern and George Washington universities in the US have developed a wireless, battery-free implantable pacemaker that uses NFC to harvest energy from an external antenna and dissolves after it is no longer needed to control a patient’s heartbeat.
The device — known as a transient pacemaker — is only 250 microns thick, weighs less than half a gram and incorporates electrodes that “softly laminate onto the heart’s surface to deliver an electrical pulse”.
“The thin, flexible, lightweight device could be used in patients who need temporary pacing after cardiac surgery or while waiting for a permanent pacemaker,” the researchers explain.
“All components of the pacemaker are biocompatible and naturally absorb into the body’s biofluids over the course of five to seven weeks, without needing surgical extraction.
“The device wirelessly harvests energy from an external, remote antenna using near-field communication protocols — the same technology used in smartphones for electronic payments and in RFID tags.
“This eliminates the need for bulky batteries and rigid hardware, including wires (or leads). Not only can leads introduce infections, they also can become enveloped in scar tissue, causing further damage when removed.”
The transient pacemaker could be used as an alternative to traditional devices which require attaching electrodes to a patient’s heart and connecting them to an external pacing box.
How it works
“Hardware placed in or near the heart creates risks for infection and other complications,” says Northwestern’s John A Rogers, who led the development team.
“Our wireless, transient pacemakers overcome key disadvantages of traditional temporary devices by eliminating the need for percutaneous leads for surgical extraction procedures, thereby offering the potential for reduced costs and improved outcomes in patient care. This unusual type of device could represent the future of temporary pacing technology.”
The functional lifespan of the device before it dissolves can also be controlled by varying the composition and thickness of its materials according to whether a patient needs it for a few days or for several weeks.
“We build these devices out of different types of safe, bioresorbable materials and in optimised architectures to ensure stable operation over a time period somewhat longer than is clinically necessary,” Rogers explains.
“We can tailor the devices to address a broad spectrum of relevant lifetimes. Transient technologies, in general, could someday provide therapy or treatment for a wide variety of medical conditions — serving, in a sense, as an engineering form of medicine.”
Rogers’ team at Northwestern University developed an NFC-powered wearable VR feedback patch in November 2019.
Next: Visit the NFCW Expo to find new suppliers and solutions